Rhinoplasty San Diego

- What is Rhinoplasty?
- Am I a Candidate?
- Benefits of Rhinoplasty
- Types of Rhinoplasty
- Your Consultation
- Procedure
- Safety
- Recovery Time
- Results
- Cost of Rhinoplasty
- Non-surgical
- FAQs
Thinking About Rhinoplasty?
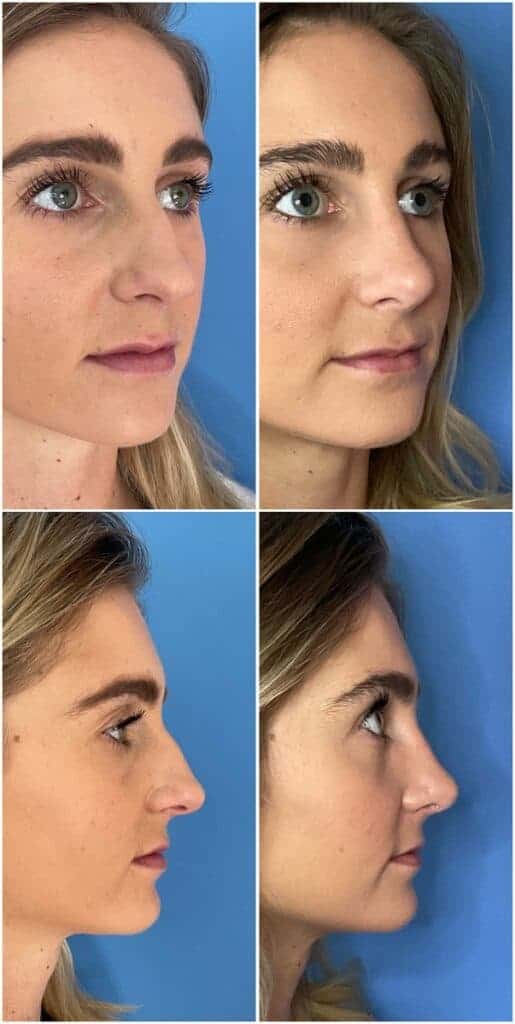
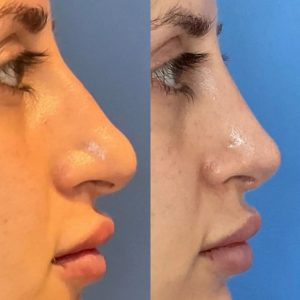
Rhinoplasty is about more than changing the nose, it’s about creating balance across the entire face. Even small irregularities like a bump, crooked bridge, or drooping tip can draw attention away from your natural features.
“One of my goals is what I call an invisible rhinoplasty. People notice that you look refreshed and balanced, but they can’t quite tell what changed. Most patients don’t want a nose that announces they had surgery. They want to look like themselves, just a better version of themselves,” says Dr. Brian Reagan.
His background includes advanced plastic surgery training at UT Southwestern in Dallas, one of the country’s most respected plastic surgery programs and internationally recognized for rhinoplasty education. He has also contributed to published rhinoplasty research and educational material related to nasal contour correction and reconstructive rhinoplasty techniques.
Patients considering rhinoplasty may also explore options such as revision procedures, functional surgery to improve breathing, or ethnic rhinoplasty focused on preserving unique features.
Why Patients Choose Dr. Reagan
Choosing the right rhinoplasty surgeon is critical. This is one of the most complex procedures in plastic surgery, requiring both technical precision and an artistic eye. Dr. Reagan stands out for his advanced training, experience, and recognized excellence.
- Board-certified plastic surgeon by the American Board of Plastic Surgery.
- Castle Connolly Top Doctor, representing the top 7% of doctors nationwide
- Named one of San Diego Magazine’s “Best Plastic Surgeons”
- Trained at UT Southwestern Medical Center, one of the top plastic surgery programs in the country
- Advanced rhinoplasty training at the Dallas Rhinoplasty Symposium
- Nationally recognized speaker and educator on rhinoplasty techniques
- Published and presented research related to rhinoplasty, nasal contour correction, and head & neck surgery topics, including work published in The Journal of Otolaryngology / Head & Neck Surgery
- Presented on nasal reconstruction and reconstructive rhinoplasty at UCSD and Scripps Memorial Hospital
- Meticulous, detail-driven approach, focused on facial balance and proportion
- Natural-looking results without the overdone appearance
Dr. Reagan has remained deeply involved in charitable and community-based surgical care throughout his career. As a former board member and volunteer surgeon for Fresh Start Surgical Gifts, he helped perform more than 200 reconstructive procedures for children and young adults with physical deformities, earning recognition with the organization’s “Health Hero Award.” He also serves on the board of The Burn Institute, supporting burn survivors and their families throughout San Diego.
“I always encourage patients to meet with more than one surgeon before making a decision. Credentials, training, and before-and-after photos are important, but they aren’t the whole story. Pay attention to how you feel during the consultation. Is the surgeon listening? Is the staff organized? Are your questions being answered? Trust and communication are just as important as surgical skill,” says Dr. Reagan.
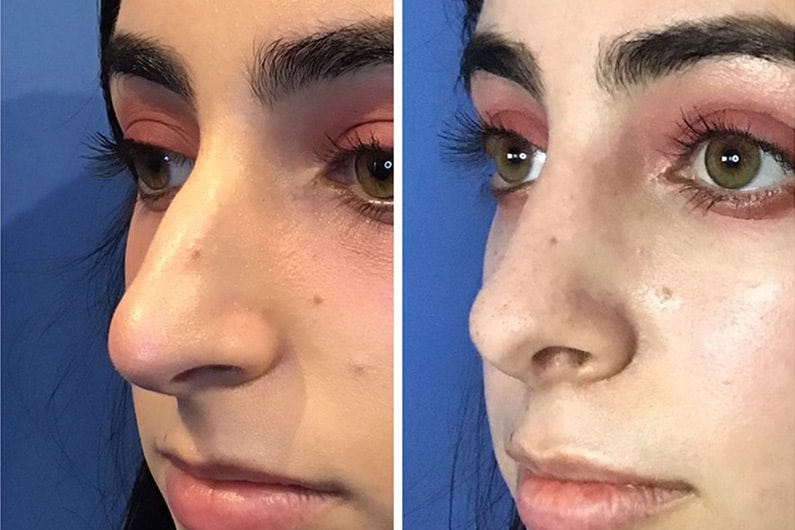
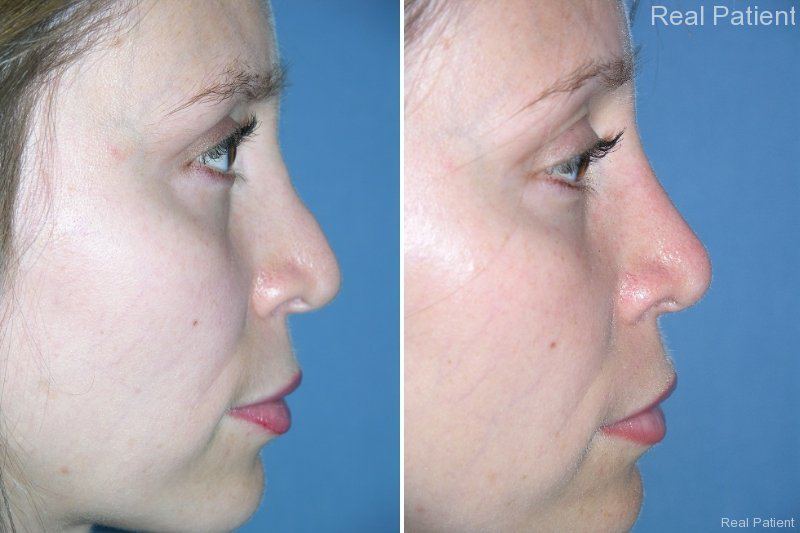
You can see the quality of his work in his before and afters and hear directly from patients through their reviews.
QUICK SUMMARY
RHINOPLASTY
*Individual patient results may vary. Examples presented are not to be interpreted as a promise or guarantee.
What Exactly is Rhinoplasty?
Rhinoplasty is a surgical procedure that modifies the shape, size and proportions of the nose to enhance facial harmony. When expertly performed, the procedure has the potential to have a tremendously positive effect on one’s appearance, confidence and quality of life.
Why Rhinoplasty Requires Specialized Experience
Rhinoplasty is one of the most technically demanding procedures in plastic surgery because even subtle changes can affect facial balance, nasal support, and breathing.
“Many plastic surgeons consider rhinoplasty one of the most challenging procedures in aesthetic surgery because you’re often working in fractions of a millimeter, yet those tiny adjustments can dramatically affect the final result. My training exposed me to some of the most advanced rhinoplasty techniques available, but one lesson has always stayed with me: the best results are often achieved through thoughtful, precise refinements rather than dramatic changes,” say Dr. Reagan.
Am I a Candidate?
You may be a good candidate for rhinoplasty if you:
- Feel self-conscious about the size, shape, or balance of your nose
- Want to improve facial harmony or profile balance
- Have breathing difficulties related to nasal structure
- Are bothered by changes from injury, genetics, or prior surgery
- Are in good overall health and do not smoke or have conditions that may impair healing
- Have realistic expectations about what surgery can achieve
“One of the biggest concerns I hear is, ‘I don’t want to look like a different person.’ Modern rhinoplasty isn’t about creating the same nose for everyone. It’s about creating a nose that fits your face. The goal is refinement, not transformation,” says Dr. Reagan.
Benefits of Rhinoplasty
Rhinoplasty offers both aesthetic and functional benefits, helping patients look better, breathe more easily, and feel more confident. While results are personalized, many patients experience improvements in the following areas:
- Improved Nose Function: Rhinoplasty offers more than the cosmetic benefits of a well-proportioned nose and flattering side profile. Nose reshaping surgery can remarkably improve the function of your nose, making it easier to breathe. Difficulty breathing through your nose affects how well you rest.
- Sleeping Better: Many patients find they get better sleep after nose surgery and feel awake and alert in the morning. When you feel well-rested, you not only feel better but look better with reduced dark circles under your eyes and a brighter appearance.
- Increased Self-Esteem: People who have surgery for cosmetic or medical reasons may experience increased self-confidence in their personal and professional life because they have a balanced, attractive facial appearance.
Techniques & Types of Rhinoplasty
Rhinoplasty can be customized in many different ways depending on your anatomy, goals, breathing concerns, and whether you have had previous nasal surgery.
There are two primary surgical approaches used to perform rhinoplasty, along with several different types of rhinoplasty procedures designed to address specific concerns.
Surgical Approaches: Open vs. Closed Rhinoplasty
Open Rhinoplasty
- Incisions are made inside the nostrils and across the columella (the strip of skin between the nostrils)
- Provides greater visibility and precision, especially for more complex cases
- May result in a small, well-hidden scar at the base of the nose
- Dr. Reagan uses this option for many procedures due to the level of control it allows
Closed Rhinoplasty
- All incisions are made inside the nostrils
- No visible external scarring
- Typically used for more limited adjustments
- Offers less direct visibility during surgery
Types of Rhinoplasty
Rhinoplasty can be customized based on both the patient’s goals and the underlying structural concerns being addressed. In addition to choosing between an open or closed surgical approach, procedures may also fall into several specialized categories.
- Cosmetic Rhinoplasty: Focused on improving the appearance, shape, and overall facial balance of the nose.
- Functional Rhinoplasty: Performed to improve breathing and correct structural issues affecting airflow, such as a deviated septum or nasal collapse.
- Revision Rhinoplasty: Designed for patients seeking correction or improvement after a previous rhinoplasty procedure.
- Ethnic Rhinoplasty: Focused on refining the nose while preserving the patient’s natural ethnic features and facial identity.
Dr. Reagan will recommend the most appropriate technique and surgical approach based on your anatomy, goals, and functional concerns.
“Patients often ask whether they need an open or closed rhinoplasty, or whether cartilage grafts will be required. In reality, these are simply tools. The right approach depends on the patient’s anatomy, goals, and functional needs. My job is to select the technique that will produce the safest, most predictable, and most natural-looking result,” says Dr. Reagan.
Common Concerns Dr. Reagan Evaluates

Your consultation with Dr. Reagan plays an important role in achieving your desired results. During this in-person visit at our San Diego/La Jolla office, he will perform a detailed evaluation of your nose.
During a consultation, Dr. Reagan evaluates more than the surface appearance of the nose. He looks at how the nasal bones, cartilage, skin thickness, tip support, bridge height, nostril shape, and breathing function work together. Common concerns may include:
- Dorsal hump or bump on the bridge
- Bulbous or drooping nasal tip
- Crooked or asymmetric nose
- Wide bridge or nostrils
- Poor tip projection or rotation
- Thick nasal skin
- Breathing obstruction or structural concerns
- Prior rhinoplasty concerns
It’s important to be open about what you don’t like about your nose and what you hope to achieve. This helps Dr. Reagan design a personalized treatment plan tailored to your goals.
Dr. Reagan’s Rhinoplasty Philosophy
Dr. Reagan believes the best rhinoplasty results should not look obvious or operated on. The goal is not to create the same nose for every patient, but to refine the features that distract from the face while preserving what makes each person unique. His approach focuses on:
- Preservation of structural support whenever possible
- Careful balance between cosmetic refinement and breathing function
- Technique selection based on each patient’s anatomy and surgical goals
“The best compliment a patient can receive is, ‘You look great, but you still look like yourself.’ That’s really what we’re trying to achieve. We make thoughtful refinements while preserving the features that make you unique,” says Dr. Reagan.
“In rhinoplasty, I strongly believe that less is often more. Small, thoughtful refinements can have a significant impact on facial harmony. The goal isn’t to create a perfect nose, it’s to create a nose that looks natural and belongs on your face.”
The Procedure & Dr. Reagan’s Approach
Rhinoplasty typically performed as an outpatient procedure under general anesthesia, meaning you’ll be able to return home the same day.
During surgery, Dr. Reagan carefully reshapes the underlying nasal structure to achieve a more balanced, natural appearance. Depending on your goals, this may involve refining cartilage, smoothing a dorsal hump, adjusting the nasal tip, or improving the size and shape of the nostrils. If needed, structural concerns that affect breathing can also be corrected at the same time.
Dr. Reagan’s approach is centered on precision, balance, and natural results:
- Focus on overall facial harmony, not just the nose
- Avoidance of overdone or “operated” appearances
- Preservation of natural structure whenever possible
- Fully customized treatment based on each patient’s anatomy and goals
- Careful balance between cosmetic refinement and functional improvement
Whether you are seeking subtle refinement, improved breathing, or revision of a previous rhinoplasty, every procedure is tailored to achieve results that look natural and feel authentic to you.
“There isn’t a one-size-fits-all approach to rhinoplasty. Some surgeons use cartilage grafts routinely, while others rarely use them. My philosophy is simple: I use grafts when they’re needed. They can be extremely helpful for improving breathing, providing structural support, or enhancing tip projection, but not every patient requires them,” says Dr. Reagan.
Once the refinements are complete, the incisions are carefully closed and a small nasal splint is placed to support the nose as it begins to heal.
View this post on Instagram
Your Safety Is Our #1 Priority
Your safety is always our top priority. While rhinoplasty is a commonly performed and generally safe procedure when performed by a qualified, board-certified plastic surgeon, all surgeries carry some level of risk.
Dr. Reagan performs surgery in an accredited surgical facility and follows strict safety protocols designed to support patient comfort, safety, and optimal outcomes throughout every stage of the process.
He will review your medical history in detail, explain potential risks, and take the time to ensure you feel fully informed and comfortable before moving forward.

Brian Reagan, MD, FACS
Dr. Brian Reagan is a board-certified plastic surgeon and founder of True Beauty San Diego Aesthetic Surgery & Medicine. Dr. Reagan is renowned for his surgical skills and commitment to patient satisfaction. Dr. Reagan has been featured on local media outlets, including ABC 10, and recognized as one of the “Best Plastic Surgeons in San Diego” by San Diego Magazine, and “Best Plastic Surgeons in La Jolla” by La Jolla Light Newspaper.

Recovery Time
Recovery after surgery is typically straightforward, with most patients returning to normal daily activities within one to two weeks.
Some swelling and bruising, especially around the eyes, is expected in the early stages but improves steadily over the first couple of weeks. While you’ll begin to see changes early on, your final results will continue to refine over several months as swelling fully resolves.
Dr. Reagan and his team will provide detailed post-operative instructions and closely monitor your healing to ensure a smooth, comfortable recovery.
RHINOPLASTY RECOVERY
Immediately After:
Patients are sent home with post operative instructions. The head should be kept elevated on several pillows.
One to Two Weeks After Surgery:
Incisions are checked. Sutures are trimmed if needed. Nasal splint is removed. Most patients are able to return to a desk job if needed – depending on how much bruising is present.
Three to Four Weeks After Surgery:
Most of the bruising and swelling should have subsided by now. Patients are typically able to begin light walking on treadmill.
One to Two Months after Surgery
At this time, the bones should be stable and more strenuous activities can be resumed. Patients are getting closer to seeing the final results.
Final Results:
On average, it typically takes 6 months to see final results with subtle improvements and healing up to a year.

*Individual patient results may vary. Examples presented are not to be interpreted as a promise or guarantee.
Your Rhinoplasty Results
The best rhinoplasty results should look natural, balanced, and appropriate for your face, not overly done or artificial. “One of the most rewarding things I hear from patients is, ‘I still look like myself, just better.’ That’s the challenge and the artistry of rhinoplasty, making meaningful improvements while preserving the patient’s natural identity,” says Dr. Reagan.
You can view real patient results in our before and after gallery and read reviews from patients to learn more about what to expect
When will I see results?
The initial swelling should subside a few weeks after your rhinoplasty, and you’ll have your first glance at your results. However, it can take up to a year for the tissues to heal and reveal your new refined nose.
How long will my results last?
Your rhinoplasty results will likely last you decades. Your face and body will change as you get older, which may cause gradual alterations in your facial appearance, including your nose. However, sun protection and leading a healthy lifestyle will help lengthen your results.
Cost of Rhinoplasty
The cost of rhinoplasty in San Diego can vary depending on the complexity of the procedure, the surgical approach required, and whether the procedure is cosmetic, functional, or revision-related. Several factors can influence pricing, including:
- Whether the procedure is primary or revision rhinoplasty
- The complexity of the nasal reshaping required
- Whether breathing or structural concerns are being corrected
- The need for cartilage grafting or reconstruction
- Whether the procedure is combined with septoplasty or other facial procedures
- Operating room, anesthesia, surgical facility, and post-operative care fees
Revision rhinoplasty and more structurally complex cases are often more time-intensive and technically demanding, which can affect overall cost.
Because every nose and surgical plan is unique, pricing can vary significantly from patient to patient. During your consultation, we will provide a detailed cost estimate outlining all associated surgical and facility fees so you fully understand what is included before moving forward.
Non-Surgical Alternatives
Liquid rhinoplasty uses hyaluronic acid fillers such as Juvederm® and Restylane® to make subtle, temporary improvements to the shape of the nose, such as smoothing small bumps or improving symmetry.
While it can be a good option for minor adjustments, it cannot reduce the size of the nose or address more complex concerns. Results are temporary and typically last several months.
For patients seeking more comprehensive, long-term results, surgical rhinoplasty remains the most effective option.
Rhinoplasty Patient Review

“I would highly recommend Dr. Reagan!!!! I recently had a rhinoplasty from him. From my first consultation to my final results I have been completely thrilled and impressed. He listened to me and did exactly what I wanted and I couldn’t be happier. He has an excellent demeanor and is very reassuring and instilled lots of confidence in me. He has a wonderful bedside manner and went far beyond my expectations. Thank you!”
Rhinoplasty FAQs

Is rhinoplasty different for men and women?
Yes. While the surgical techniques may be similar, the aesthetic goals are often different. Male rhinoplasty typically focuses on maintaining stronger, more defined nasal features, while female rhinoplasty often emphasizes softer refinement and facial balance.
Dr. Reagan customizes every rhinoplasty procedure based on facial structure, skin thickness, anatomy, and the patient’s personal goals to achieve natural-looking results that complement the face.
What factors affect rhinoplasty results?
Several factors can influence rhinoplasty results, including skin thickness, cartilage strength, nasal anatomy, healing response, age, and whether the procedure is primary or revision rhinoplasty.
During your consultation, Dr. Reagan carefully evaluates each of these factors to develop a personalized surgical plan designed to support long-term structural integrity, facial balance, and natural-looking results.
How long does swelling last after rhinoplasty?
Most noticeable swelling improves within the first few weeks, and many patients return to work or normal activities within 1–2 weeks. However, subtle swelling, particularly around the nasal tip, can continue improving for several months.
Final rhinoplasty results typically develop gradually over 6–12 months as the nose refines and tissues fully heal.
Can rhinoplasty improve breathing?
Yes. In addition to cosmetic improvement, rhinoplasty can help correct structural issues that interfere with breathing, such as a deviated septum, internal valve collapse, or nasal asymmetry caused by injury or prior surgery.
Functional rhinoplasty techniques can improve airflow, breathing comfort, and overall nasal support while also enhancing appearance.
What procedures can be combined with rhinoplasty?
Rhinoplasty is often combined with procedures like chin augmentation, eyelid surgery, or facial rejuvenation treatments to enhance overall facial balance.
Combining procedures can also reduce overall recovery time by addressing multiple concerns at once.
What types of rhinoplasty are available?
Rhinoplasty can be customized to address a wide range of cosmetic and functional concerns. Specific concerns that can be addressed include dorsal humps, drooping nasal tips, wide nostrils, asymmetry, trauma-related deformities, and structural breathing issues.
Will my nose still look natural after rhinoplasty?
Dr. Reagan focuses on creating natural-looking rhinoplasty results that complement your facial features rather than dramatically changing your appearance. The goal is typically to refine balance and proportion while preserving facial character and avoiding an overdone appearance.
Schedule Your Consultation Today
If you’re considering rhinoplasty, a consultation with Dr. Reagan is the first step in understanding your options and what’s possible for your unique features.
Contact our San Diego office at (858) 454-SKIN (7546) or email us to schedule your visit.
Patient Reviews & Testimonials

“Dr. Reagan is a wonderful combination of excellent technician, clear communicator, and artist. He clearly explained all procedures, options, and risks. I wanted a result that would look amazing, and at the same time be conservative and look totally natural. Dr. Reagan surpassed all expectations and I’m absolutely thrilled with the result. He is a remarkable physician. A bonus is the lovely office and staff.”